Bariatric Surgery Frequently Asked Questions
What Is Bariatric Surgery?
Bariatrics is the branch of medicine that deals with the study, treatment, and prevention of obesity. Bariatric surgery is any surgical procedure performed for the purpose of losing weight or treating obesity. This is generally accomplished through the implantation of a medical device (such as Lap-Band), removing a portion of the stomach, or reducing the size of the stomach. Dr. Davtyan at The Weight Loss Surgery Center of Los Angeles, frequently performs two of the most prevalent bariatric surgery procedures: Lap-Band and gastric sleeve. When you have a consultation with Dr. Davtyan, he will assess and recommend whether Lap-Band or gastric sleeve is the more suitable option for you.
What Is BMI Or Body Mass Index?
Your BMI, or body mass index, is a measurement of your weight in relation to your height. It’s used to assess how far your weight deviates from what is considered to be optimal for a person of your height. It’s a reliable indicator of how much excess fat you have, but it doesn’t take into account other factors that can contribute to your weight, like muscle and bone structure. As such, it’s an important screening tool, but most doctors will also provide other, more detailed tests to determine if your extra weight is a true health risk.
What Qualifies A Person As Being Overweight, Obese, Or Morbidly Obese?
The U.S. Center for Disease Control and Prevention uses the following chart to determine an adult’s general weight status, based on their BMI:
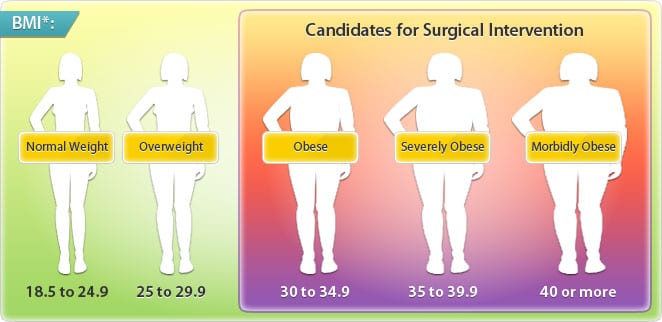
How Much Weight Can I Expect To Lose With Bariatric Surgery?
The amount of weight you lose will depend on the type of bariatric surgery performed, as well as your commitment to maintaining a healthy lifestyle moving forward. With that said, most patients can expect to lose approximately one to three pounds a week over a period of 12 to 24 months.
Will Insurance Cover My Surgery?
Most major insurance companies cover bariatric surgery, as long as you meet their requirements. At Dr. David Davtyan’s office, we routinely work with our patients’ insurance providers to help them get approved for the care they need.
Learn More About Insurance Coverage
How Do I Get Started?
Your weight loss journey begins with an initial complimentary consultation with Dr. David Davtyan. During that meeting, he will listen closely to your weight loss challenges, concerns, and medical history, before composing a custom treatment plan designed to help you lose the weight for good and reclaim your health. Feel free to check our bariatric surgery options section to learn more about different surgical procedures, their efficacy, and the risks.
How long does it take to recover from a Gastric Sleeve procedure?
The Gastric Sleeve procedure usually lasts 1 to 2 hours. The post-op recovery in the recovery room is usually a couple of hours. I typically keep my patients overnight for their comfort and discharge them home the next morning after an X-Ray confirms that the sleeve looks great without any narrowings (strictures) or leaks from the staple line. The full recovery at home varies from person to person, but it typically takes a few days since the surgery is done laparoscopically (i.e., minimally invasive). The return to work also varies from person to person, as well as the degree of physical activity involved in their job.

Are there any risks following a Gastric Sleeve surgery?
Any kind of surgical procedure can have risks associated with it. In surgery, we typically divide the risks into those associated with anesthesia and any surgical intervention on one side and on the other risks related to the specific procedure that is being performed. One should also understand that the risks are particularly elevated in any individual with morbid obesity as well as individuals who are undergoing revisional (i.e., repeated) weight loss operations. Hence, it is extremely important that patients do everything in their power to try to reduce their weight prior to surgery. Gastric sleeve, also known as Sleeve Gastrectomy, carries all the typical risks associated with general anesthesia such as heart attack, stroke, blood clots, pulmonary embolism (blood clots that travel from leg veins to the lungs), and many others. To minimize these risks, I will routinely perform a very thorough evaluation of the patient, obtain clearance for surgery from my internal medicine, cardiology, or pulmonary medicine colleagues as well as administer blood thinners during and after the operation to decrease the risk of blood clots and antibiotics to decrease the risk of infection. During Sleeve Gastrectomy, we remove a large part of the stomach. To do that we must first detach all of the blood vessels that come to that part of the stomach, after which we separate that part of the stomach with a special instrument that staples and divides at the same time from the thin, banana sized/banana shaped, sleeve of the stomach, which we leave behind. As a result, the most common complications are related to the division of those blood vessels which can bleed, and the placement of a 30 cm long staple line, which can leak and cause peritonitis (infection of the abdomen) and sepsis (infection of the blood). See the Gastric Sleeve Video and Illustration. To find out more about all possible risks and benefits of the Gastric sleeve, call us toll-free at 1(877) 9-BESLIM.
What lifestyle changes are required following a weight loss surgery?
Any weight loss surgery is only a tool or a weapon for the patients to use in their battle against excess weight. Based on the determination and the ferocity of the patient in his or her fight against obesity, the outcomes will range from excellent to poor. There is no “perfect” weight loss operation. They all have their pros and cons. Fortunately, all outcomes can be tremendously improved by the patients if they implement significant lifestyle changes. To put it in very simple terms, weight loss is about making sure that a person burns more calories than he or she consumes. Therefore, any post-bariatric surgery patient should become an expert on counting calories. In my practice, I notice that many patients find it easy to add up the calories of the food they ate throughout the day if they take pictures of their meals and add them up later in the evening when they have time to sit on the couch and look up on the internet (iPhone has many apps) the caloric value of every meal. All weight loss surgeries work by limiting caloric intake. The increase of caloric expenditure (calories you burn) is entirely up to each individual. Every bariatric surgery patient should at least count their steps and try to increase the number of daily steps up to 10,000 (iPhone’s health app has a built-in pedometer) as well as enroll at a local gym and adopt a comfortable exercise routine, preferably with a personal trainer to prevent any injury.
Is it possible to achieve an ideal body weight after gastric banding?
The answer is yes. It is possible to get to an ideal body weight after gastric banding surgery. Most people lose about half of the excess weight after this procedure during the first year. Maximum weight loss with the Lap Band is usually achieved in 3 to 4 years. Compared to other procedures, Lap-Band induced weight loss is more gradual and better tolerated by the body (less hair loss or nutritional deficiencies). Most weight loss operations will help patients achieve their desired weight, but the maintenance of that achievement will depend on that patient’s ability to implement the necessary lifestyle changes to maintain a low caloric intake/high caloric expenditure ratio.

After losing weight, can I have the Lap-Band removed?
Many patients ask whether they can have the Lap Band removed after they have achieved their goal weight. While it is very easy to remove the Lap Band, it is meant to stay in place for as long as it is functioning properly and is helping the patient to lose or maintain weight. In my experience, the removal of the Lap Band or even its deflation is associated with weight regain which sometimes can be significant and irreversible.
How do I know if my Lap-Band needs an adjustment?
The decision to inflate or deflate the Lap Band (Lap Band adjustment) I always make together with the patient. Typically, I will recommend inflating the band if, in spite of the patient’s best efforts, there is no weight loss for 2 weeks or any weight regain. The recommendation to deflate is frequently related to the Band being too tight, patients getting pregnant (which is very common in young women after major weight loss), and patients traveling to extremely high altitudes or remote locations where access to care may be limited.